Effect of a Technology-Supported Physical Activity Intervention on Health-Related Quality of Life and Sleep in Cancer Survivors: A Randomized, Controlled Trial
Abstract
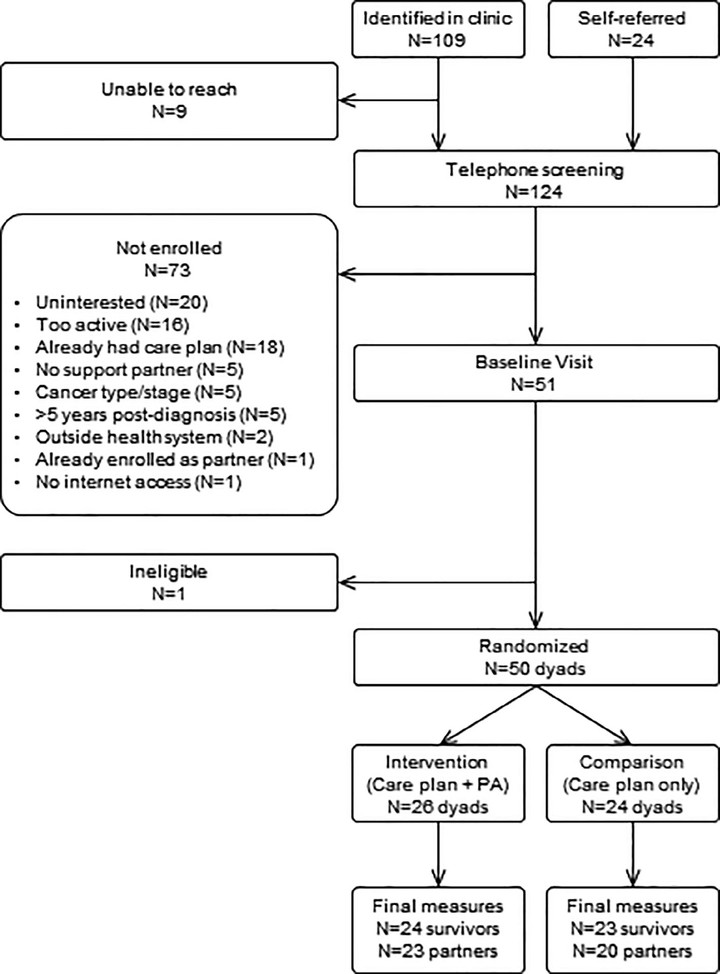
Objectives This pilot trial tested the effect of adding a multi‐level, technology‐based physical activity intervention module to a standard survivorship care plan for breast and colorectal cancer survivors. The objective of this analysis was to determine whether the physical activity module improved health‐related quality of life, sleep, and factors key to lasting behavior change (eg, social support, self‐efficacy). Methods Breast and colorectal cancer survivors (n = 50) were enrolled alongside a support partner. Survivors were assigned to receive a standard survivorship care plan either alone or augmented by a 12‐week multi‐component physical activity module. The module included a Fitbit tracker (with the physical activity data integrated into the electronic health record for clinician review) and customized email feedback. Physical activity was measured using the ActiGraph GT3X+. Psychosocial outcomes included the SF‐36, FACT, ISEL, PROMIS sleep measures, and physical activity beliefs. Data were analyzed using linear mixed modeling. Results Cancer survivors were aged 54.4 ± 11.2 years and were 2.0 ± 1.5 years from diagnosis. Relative to comparison, the intervention was associated with moderate‐to‐large improvements in physical health (effect size: d = 0.39, 95% CI = 0.0, 0.78), mental health (d = 0.59, 95% CI = 0.19, 0.99), sleep impairment (d = 0.62, 95% CI = −1.02, −0.22), and exercise self‐efficacy (d = 0.60, 95% CI = 0.20, 1.0). Conclusions The intervention delivered meaningful improvements in survivors’ quality of life, social support, and sleep impairment. If replicated in a larger sample, adding a technology‐supported physical activity module to survivorship care plans may be a practical strategy for supporting healthy survivorship.